Lacrimal duct diseases
ICD codes: H04 What are ICD codes?
Lacrimal duct diseases include both the lacrimal glands and draining tear ducts of the lacrimal apparatus. In this article, you will learn more about the symptoms and treatment of an obstruction of the lacrimal ducts and inflammation of the lacrimal glands.
At a glance
- Medical practitioners use the terms lacrimal duct stenosis or dacryostenosis for an obstruction of the draining tear ducts.
- As a result, tear fluid is no longer able to flow sufficiently into the nose via the lacrimal ducts.
- About 6% of children enter the world with a congenital lacrimal duct obstruction.
- The obstruction usually disappears within the first few months of life if it is treated – especially with massages.
- An inflammation of the lacrimal gland is called dacryoadenitis.
- Causes can be bacteria, viruses or another disease. Sometimes the cause is unknown.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
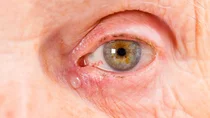
What are lacrimal duct diseases?
The lacrimal apparatus includes the structures around the eyes and nose which produce and discharge tears. Important structures of the lacrimal apparatus are:
- the (primary) lacrimal gland, which is located in the eye socket laterally above the eye and produces tear fluid
- one lacrimal point per eyelid, with each one forming a “drain” for the tear fluid into a lacrimal duct
- the lacrimal ducts, which discharge the lacrimal fluid into the lacrimal sac
- the lacrimal sac, which catches the lacrimal fluid, collects it and finally guides it into the nasal cavity
Diseases and disorders of the lacrimal ducts can:
- be congenital, referred to as a congenital lacrimal duct obstruction (dacryostenosis)
- be caused by bacteria or viruses; these are commonly a lacrimal gland inflammation (dacryoadenitis)
- develop as a result of an injury or if a foreign body obstructs a lacrimal duct
- occur without a recognizable cause, referred to as an idiopathic lacrimal duct disease
Around 6% of newborns have a congenital lacrimal duct obstruction. But they can also develop it during their life, for instance due to inflammations.
A lacrimal gland inflammation can occur both after an infection of the eye and as a result of another disease, such as an infection with the Epstein-Barr virus – the pathogen of glandular fever.
Important: While an acute lacrimal gland inflammation is usually painful, there is not normally any pain during a chronic inflammation of the lacrimal glands.
What are the symptoms of lacrimal duct diseases?
The symptoms of lacrimal duct diseases depend on the cause and affected area. The symptoms can thus be very different.
Signs of a congenital lacrimal duct obstruction
With a congenital obstruction of the lacrimal ducts (dacryostenosis), an unopened mucous membrane usually impedes the discharge of lacrimal fluid into the nose through the nasolacrimal canal. The result is that the eye waters frequently or constantly. With slight pressure on the lacrimal sac, a lacrimal reflux and visible secretion discharge may occur.
Important: A rare complication of a lacrimal duct obstruction can be when a lacrimal sac inflammation (dacryocystitis) with symptoms like pain and fever develops. In newborns, an acute inflammation of the lacrimal sac is an emergency that must be treated immediately.
Signs of an acute lacrimal gland inflammation
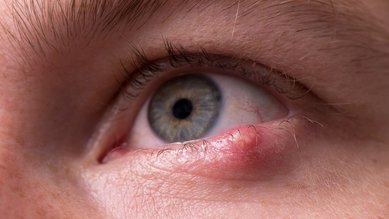
An acute inflammation of the lacrimal ducts (dacryoadenitis) is usually caused by an infection and normally occurs on one side. It can be detected by redness and an occasional severe swelling on the upper lateral margin of the eye socket. As a result, the outer area of the eyelid may be pushed downward. With an inflammation caused by bacteria, pus may form.
Other possible symptoms are:
- scabs and lachrymation (tears flowing)
- lymph node swelling
- fever and malaise
- a preceding or concurrent conjunctivitis
Signs of a chronic lacrimal gland inflammation
A swelling on one or both sides of the upper lateral margin of the eye socket, which does not usually cause any pain, is typical for a chronic inflammation of the lacrimal glands. This swelling usually grows more slowly than with an acute inflammation.
What are the causes of lacrimal duct diseases?
The causes of a lacrimal duct disease are determined by the form of the disease – and thus by whether there is an obstruction of the lacrimal ducts or an inflammation of the lacrimal glands.
Causes of congenital lacrimal duct obstruction
The cause of a congenital lacrimal duct obstruction (dacryostenosis) is usually a small fold in the nasolacrimal canal at the junction with the nasal mucous membrane, known as Hasner’s fold. If this fold does not open by itself after birth as it is meant to, the discharge of tears into the nose is obstructed or completely blocked.
Causes of an acute lacrimal gland inflammation
An acute inflammation of the lacrimal glands (dacryoadenitis) normally develops as a result of a bacterial or viral infection. The pathogens get into the lacrimal gland through either the conjunctiva, the adjacent skin or an injury. Systemic infections that spread through the bloodstream in the body may also cause an acute inflammation. In particular, these include infections with influenza viruses, the Epstein-Barr virus, the mumps virus, the varicella zoster virus, certain bacterial strains and – much more rarely – particular fungi.
Causes of a chronic lacrimal gland inflammation
A chronic inflammation of the lacrimal glands is often associated with another chronically inflammatory disease. These include for instance the lung disease sarcoidosis, the vascular disease Wegener’s disease or the gastrointestinal disease Crohn’s disease. However, doctors are unable to find any clear cause for many people with chronic lacrimal gland inflammation.
How common are lacrimal duct diseases?
A congenital lacrimal duct obstruction occurs in about 6% of newborns and is the most common cause of persistent tears in the eyes of infants and small children.
It is not known how often lacrimal gland inflammations occur. However, they are rare overall and generally occur in children, adolescents and young adults.
A chronic inflammation of the lacrimal glands, which is associated with an autoimmune disease like Crohn’s disease, occurs more commonly in women than men, because more women generally have autoimmune diseases.
How are lacrimal duct diseases diagnosed?
Lacrimal duct diseases are usually easy to recognize. An obstruction of the lacrimal ducts (dacryostenosis) is typically expressed by watery eyes, tears and sometimes a secretion discharge. With dacryoadenitis, the lacrimal gland occasionally swells up severely.
If doctors detect such signs during an examination, they can initiate further diagnostic measures if necessary.
Congenital lacrimal duct obstruction
Doctors ask the child’s parents about abnormalities such as increased lachrymation and examine the child’s eyes – to also rule out other eye diseases. As a general rule, a diagnosis can be made after that.
For additional diagnostic confirmation, doctors can carry out a standardized test to assess lachrymation – for example the so-called Schirmer’s test. In the course of this, a test strip made of litmus paper is suspended in the conjunctival sac to assess the amount of tears produced. The conjunctival sac is a mucous membrane. This begins at the edge of the eyelid and covers the rear surface of the eyelids facing the eyeball.
When necessary, they can also examine the backlog of lacrimal fluid with a small needle that is carefully inserted into the lacrimal points of the lower eyelid after local anesthesia.
Acute and chronic lacrimal gland inflammation
When there is a swelling of the lacrimal glands that occurs due to a viral disease, no other examinations are normally necessary.
Doctors carry out an expanded diagnosis in particular if:
- the cause of the lacrimal gland inflammation is unclear
- it is not clear whether it is actually an inflammation of the lacrimal glands or another disease
- a treatment is not showing the desired success
- older adults are sick
- both eyes are affected
With an examination of the blood for example, certain antibodies can be detected that shed light on whether an autoimmune disease is present.
Imaging techniques like magnetic resonance imaging (MRI) can make an enlargement or change of the lacrimal gland visible. Another possibility is to do a biopsy, meaning that a tissue sample is taken and examined.
How are lacrimal duct diseases treated?
The treatment options vary depending on the type of lacrimal duct disease. They range from a mere medical follow-up to medical measures and surgery.
Treatment of a congenital lacrimal duct obstruction
In newborns, obstruction of the lacrimal ducts (dacryostenosis) can often be easily solved within the first weeks of life. To treat a congenital obstruction, diligent eyelid hygiene is recommended along with regular massage of the affected lacrimal ducts and, if necessary, the lacrimal sac. Both can be carried out by parents themselves after expert guidance. A lacrimal duct obstruction can thus most often be solved within weeks or a few months.
If a pus-filled secretion accumulates in the eye region, it is often an indication of the lacrimal sac being colonized by bacteria. In that case, the doctor will additionally prescribe antibiotics that counteract these bacteria.
If the lacrimal duct obstruction is present after the age of six months as well, doctors examine the lacrimal ducts with a special probe or needle. In the process, the lacrimal ducts can be carefully rinsed with excess pressure.
If massages, medications and rinses remain unsuccessful, a surgical intervention may be required. In the course of this, the doctor creates a connection between the nasal cavity and lacrimal sac. This makes it possible for lacrimal fluid to flow off into the lacrimal sac in spite of closed lacrimal ducts.
Treatment of an acute lacrimal gland inflammation
An acute lacrimal gland inflammation (dacryoadenitis) caused by viruses usually heals by itself within 4 to 6 weeks. If bacteria are the cause of the inflammation, it is sensible to take antibiotics – bactericidal drugs. If a pus-filled pocket (abscess) forms, it may be necessary to have this opened during a small operation.
Doctors can prescribe corticosteroids against the swelling of the lacrimal gland. That is a group of anti-inflammatory drugs.
Treatment of a chronic lacrimal gland inflammation
A chronic inflammation of the lacrimal glands can often be traced back to another disease. It is therefore important to treat both diseases. To help the swelling in the lacrimal gland go down, corticosteroids are used as for acute inflammation.
- DynaMed (Internet), Ipswich (MA). Nasolacrimal Duct Obstruction. EBSCO Information Services. Record No. T113767. Aufgerufen am 09.07.2021.
- Patel R, Patel BC. Dacryoadenitis. [Updated 2021 June 23]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Aufgerufen am 09.07.2021.
- UpToDate (Internet). Approach to the child with persistent tearing. Wolters Kluwer 2018. Aufgerufen am 09.07.2021.
- UpToDate (Internet). Congenital nasolacrimal duct obstruction (dacryostenosis) and dacryocystocele. Wolters Kluwer 2019. Aufgerufen am 09.07.2021.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at: