Cirrhosis of the liver
ICD codes: K74 What are ICD codes?
Cirrhosis of the liver is a process in which liver tissue is destroyed and replaced by connective tissue that has no function. If this process continues, the liver may become entirely shrunken. Long-term alcohol consumption and chronic viral hepatitis are two common causes of liver cirrhosis.
At a glance
- With cirrhosis of the liver, intact liver tissue is destroyed and replaced by connective tissue (scar tissue) that has no function.
- Cirrhosis of the liver often develops unnoticed over many years.
- It can have various causes, including long-term alcohol consumption and chronic inflammation of the liver.
- Treatment aims to halt or slow progression of the scarring and to avoid complications.
- If scarring of the liver tissue is at a very advanced stage, a liver transplant may be the only treatment option available.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is cirrhosis of the liver?
With cirrhosis of the liver, the liver tissue is gradually destroyed and transformed into gnarled connective tissue (scar tissue) that has no function. This scarring process can continue until the liver becomes entirely shrunken. The connective tissue is unable to perform the functions of normal liver cells. In the long term, this leads to liver failure.
Cirrhosis of the liver is most commonly caused by uncured liver diseases, such as chronic viral hepatitis or by liver damage caused by consuming alcohol over many years.
Cirrhosis of the liver usually develops unnoticed over many years because it often remains without symptoms for a long time.
The disease is frequently not detected until complications arise. Some of these complications can be life-threatening.
What are the symptoms of liver cirrhosis?
Cirrhosis of the liver can develop over several years without causing symptoms. Up to 40% of those affected by the disease don’t initially notice any changes.
Early symptoms of the disease include:
- tiredness and fatigue
- weight loss
- loss of appetite
- itchy skin
Additional symptoms develop as the cirrhosis progresses:
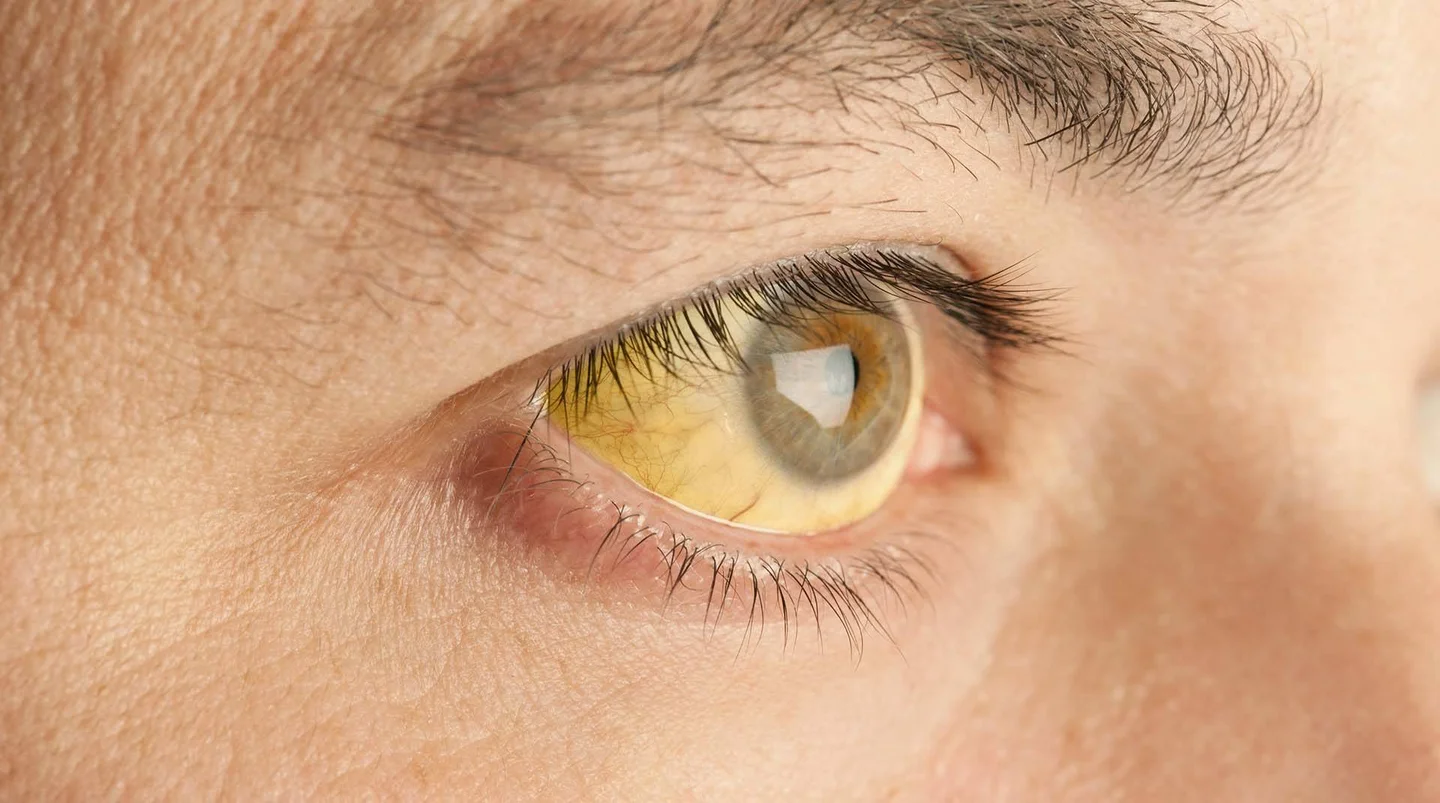
- Jaundice: a yellowing of the skin, mucus membranes and eyeballs
- Severe itching
- Signs of liver disease on the skin: typical skin changes include reddening of the palms of the hands (palmar erythema) and spider nevi/spider angiomas, which appear as red dots surrounded by web-like or star-shaped patterns of tiny blood vessels. These appear on the face and chest in most cases.
- Painful cracks at the corners of the mouth and visibly red, shiny lips (chapped lips)
- Increased estrogen levels: in men, this can result in breast enlargement, loss of hair on the abdomen (abdominal baldness) and reduced sex drive. Meanwhile, women may experience irregular menstrual periods.
What are the causes of liver cirrhosis?
The most common causes of cirrhosis of the liver include:
- a persistently high level of alcohol consumption
- non-alcoholic fatty liver disease
- chronic viral diseases of the liver, especially hepatitis B and hepatitis C
Other causes are also possible, such as:
- autoimmune hepatitis – a disease in which the immune system attacks healthy liver cells
- Wilson’s disease (copper buildup in the liver) – a rare hereditary metabolic disorder
How can liver cirrhosis be prevented?
Consuming large volumes of alcohol on a regular basis is a common cause of liver cirrhosis. Therefore, the most important preventive measure is to reduce alcohol consumption to a safe level.
The German Centre for Addiction Issues (Deutsche Hauptstelle für Suchtfragen) recommends that women shouldn’t consume more than 12 grams of pure alcohol per day. This is equivalent to a small beer (0.3 liters) or a small glass of wine (0.125 liters), for example. Men should consume no more than 24 grams of pure alcohol daily.
Another common cause of liver cirrhosis is a chronic inflammation of the liver due to an infection with hepatitis viruses.
Vaccines against hepatitis A and B are available. Using condoms reduces the risk of contracting hepatitis viruses during sex.
How does liver cirrhosis progress?
Doctors distinguish between compensated and decompensated liver cirrhosis.
With compensated cirrhosis, no major complications have developed thus far. This cirrhosis often goes unnoticed initially.
With decompensated cirrhosis, scarring of the liver has progressed to the extent that severe or even life-threatening complications have developed.
These include:
- esophageal varices, i.e. rupturing and bleeding of enlarged veins in the esophagus
- a buildup of fluid in the abdomen (ascites) and spontaneous bacterial infection of the lining of the abdomen (peritonitis)
- liver cell cancer
- hepatic encephalopathy
Hepatic encephalopathy is a brain function disorder. Due to cirrhosis, the liver can no longer break down toxic substances in the blood to a sufficient degree. As a result, the level of toxic substance in the body rises. This also affects the brain. Early symptoms are slight confusion, slowed thought processes and mood swings. In many cases, people also become sleepy more often or seem listless. Shaking hands and changes in handwriting are noticeable. In the worst case scenario, the person loses consciousness – this is known as liver coma or hepatic coma. When this happens, the person shows no response to being spoken to or to pain.
How is liver cirrhosis diagnosed?
If cirrhosis of the liver is suspected, a physical examination can reveal initial indications of the disease. An enlarged liver is one possible sign of cirrhosis.
Doctors also look for signs of liver disease on the skin, i.e. typical skin changes that frequently occur with liver diseases.
Imaging techniques are usually also used for diagnosis. These include transient elastography. This painless procedure is based on ultrasound waves. It indicates whether the liver tissue is already scarred and to what degree. However, examinations are not always adequate for diagnosis in the early stages of cirrhosis. It may also be necessary to take a tissue sample (biopsy). This involves using a fine hollow needle to remove liver tissue for analysis in a laboratory.
As well as diagnosing cirrhosis of the liver, it is also important to assess the severity of the disease and whether possible complications have developed. It is also important to determine the causes of the cirrhosis for the purpose of treatment.
A blood test can help assess the severity of the disease. It also serves to detect the presence of possible infections with hepatitis B and hepatitis C viruses.
How is liver cirrhosis treated?
The treatment of liver cirrhosis aims to halt or at least slow the progression of the disease.
For this purpose, the cause of the liver cirrhosis is treated where possible – for example, with antiviral therapy in the case of viral hepatitis.
Important: Medication should only be used when absolutely necessary. Doctors will also check to determine whether dosage needs to be adjusted.
In general, a healthy lifestyle can help to reduce liver damage – it is essential to stop drinking alcohol, taking drugs and smoking. This also applies even if the cirrhosis hasn’t been caused by alcohol. Patients who are overweight are advised to lose weight.
Some complications of cirrhosis of the liver can be life-threatening. It is therefore essential to detect and treat complications at an early stage and to prevent further complications from occurring.
For example, antibiotics may be prescribed on a precautionary basis with the aim of avoiding a spontaneous bacterial infection of the lining of the abdomen (peritonitis).
If cirrhosis is at an advanced stage and the liver is extensively scarred, a liver transplant may be considered.
- DynaMed [Internet]. Ipswich (MA). Cirrhosis of the Liver. EBSCO Information Services. Record No. T114078. 1995 (2018). Aufgerufen am 04.03.2022.
- UpToDate [Internet]. Cirrhosis in adults: Overview of complications, general management, and prognosis. Wolters Kluwer 2021. Aufgerufen am 04.03.2022.
- UpToDate [Internet]. Noninvasive assessment of hepatic fibrosis: Ultrasound-based elastography. Wolters Kluwer 2021. Aufgerufen am 04.03.2022.
- UpToDate [Internet]. Pathogenesis of hepatic fibrosis. Wolters Kluwer 2022. Abgerufen am 04.03.2022.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at: