Cancer screening: what examinations are available?
With screening, cancer or a precursor of cancer can be detected early, even before it causes symptoms. The prospects of successful treatment and thus healing and survival are thereby increased. Which examinations are covered by health insurance companies? And what can they achieve?
At a glance
- Cancer screening examinations are used to discover early forms of cancer and possibly cancer precursors before they cause symptoms.
- Participation in cancer screening is voluntary – because every early detection can have drawbacks as well as benefits.
- Both statutory and private health insurance funds bear the costs of examinations regulated by law.
- Currently, the costs for breast cancer, bowel cancer, prostate cancer, cervical cancer and skin cancer screenings are covered by the health insurance funds.
- Additional cancer screening examinations are also available – these form part of what are known as individual health services (in German: individuelle Gesundheitsleistungen, abbreviated to IGeL). They are not paid for by the statutory health insurance funds. For the most part, it is unclear whether they actually have a benefit for patients.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is cancer screening?
Cancer screening serves to detect cancer at a stage when it has not yet caused symptoms – such as pain, bleeding, or palpable lumps. Cancer screening examinations seek to detect a previously unnoticed malignant tumor at a very early point in time. This means that the cancer can be treated earlier and often more successfully too. As a result of this, the prospects of healing can be increased. Furthermore, less invasive therapies are sometimes possible.
Cancer screenings are examinations used to detect the preliminary stages of a cancer – such as initial changes in tissue. Such examinations are so far only possible with a few types of cancer, for example bowel cancer or cervical cancer. Removing benign intestinal polyps during a colonoscopy can thus help prevent the development of malignant bowel cancer.
In Germany, various early detection screenings for certain cancers were introduced as early as 1971 for all people with statutory health insurance. Since then, the offered preventive and early detection measures have been developed further based on current scientific knowledge.
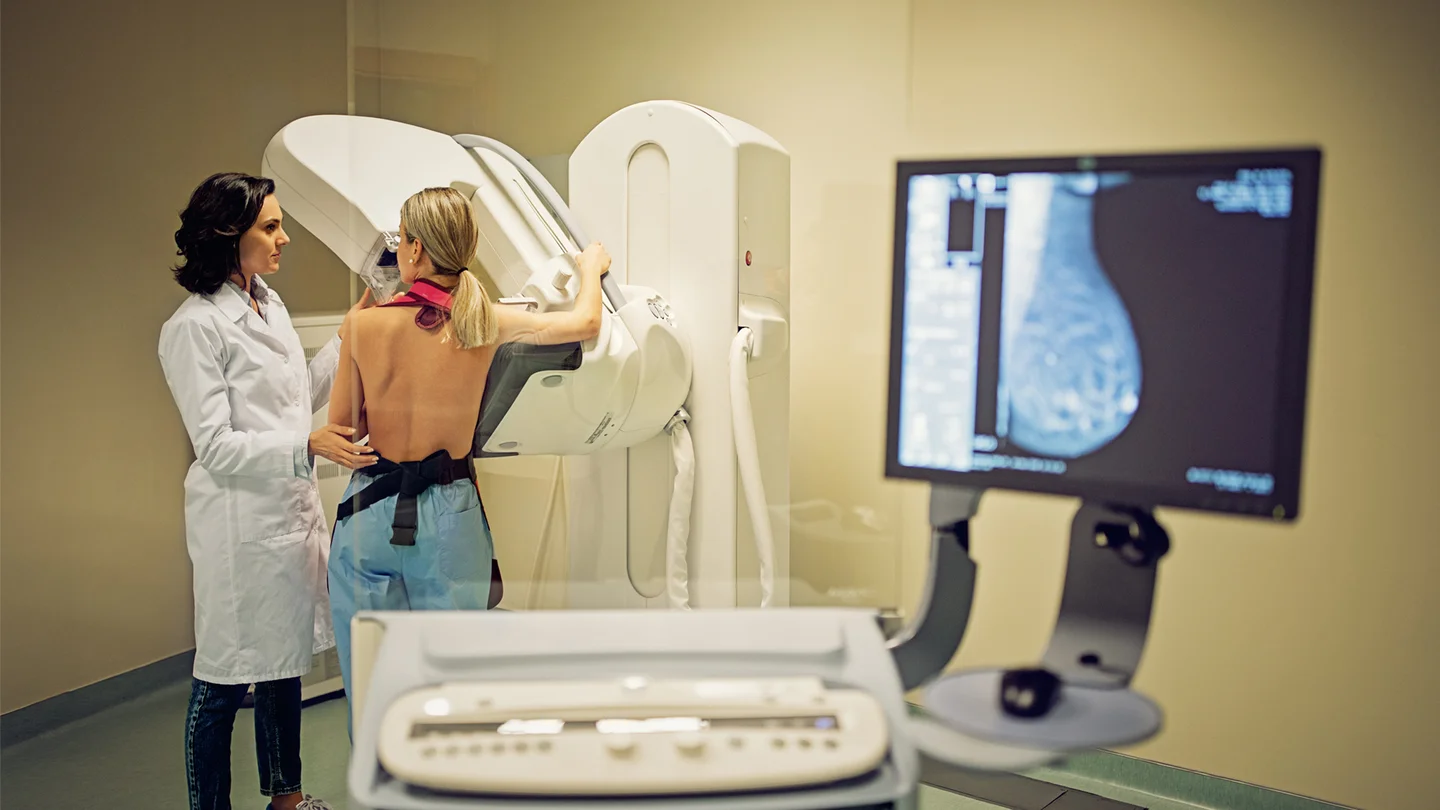
For example, a nationwide mammography screening program began in Germany in 2009 for the early detection of breast cancer. Women aged 50 to 69 are invited to get a mammogram (X-ray of the breast) every two years. Since July 2024, women up to the age of 75 can also attend mammography screening. However, they must register for this themselves beforehand.
Meanwhile, the statutory health insurance funds also invite people personally and in writing to get bowel cancer and cervical cancer screening at regular intervals. Along with the invitations, insured people are given comprehensive and balanced information about the benefits and risks of the particular examination at the same time. The invitations are used to provide customized information to insured people. But the examination can also be claimed without a prior invitation as soon as the appropriate age has been reached.
Video What is cancer?
The video below explains when doctors talk about cancer and how cancer occurs.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
What examinations are offered as part of statutory cancer screening?
Currently, the health insurance funds bear the costs of the following examinations for cancer screening and prevention:
Cervical cancer screening
- annual examination of the external and internal genitalia from the age of 20 years
- annual cervical smear for women aged 20 to 34 years
- cervical smear and human papillomavirus (HPV) test for women aged 35 years and up, every three years, provided the examination does not give any indications of cell changes and/or an HPV infection
Breast cancer screening
- annual breast exam and instructions on self-examination for women aged 30 years and over
- mammography of both breasts for women aged 50 to 75 years, every two years
Skin cancer screening
- complete physical examination of the skin for women and men aged 35 years and up, every two years for the early detection of malignant melanomas and non-melanoma skin cancer
Prostate cancer screening
- annual prostate exam for men aged 45 years and over
Bowel cancer screening
- initial colonoscopy for women and men aged 50 years and over – if results are normal, this can be repeated after ten years but if changes such as intestinal polyps are found, the examination will be repeated sooner.
- if an individual does not avail of the colonoscopy: a test is offered every 2 years to detect hidden blood in the stool
Assessment of the offered tests in terms of their benefits and risks depends on the type of cancer and examination method.
How are cancer screening and prevention regulated?
The German Federal Joint Committee (Gemeinsamer Bundesausschuss, G‑BA) decides which cancer screening examinations are included in the benefits catalog of the statutory health insurance funds. This decision-making body of our health system also determines who has a claim to these examinations, at what age and in which time intervals.
Both statutory and private health insurance funds bear the costs of examinations regulated by law as a rule. Those with insurance can freely decide whether they want to avail of the examinations. Participation is thus voluntary.
There are also examinations and tests that are offered in medical practices, but are not part of the statutory screening program. The costs are not borne by the statutory health insurance funds. This means that anyone who wants to avail of these examinations has to cover the cost themselves. They are also called individual health services (in German: individuelle Gesundheitsleistungen, abbreviated to “IGeL”). Examples include an ultrasound examination of the ovaries and prostate or determination of some values from the blood or other bodily fluids in the laboratory. Individual health services are often medical measures for which there is no sufficient proof of their benefits or which have not yet undergone a benefit assessment.
What are the possible advantages and drawbacks of screening?
As a general rule, participation in cancer screening is voluntary. There is no time pressure, so it is possible to calmly learn about the advantages and drawbacks of cancer screening.
Advantages of cancer screening
Participation in cancer screening can result in cancer being prevented (in the best case) or discovered at a very early stage. An early start to treatment increases the prospect of healing and decreases mortality. Furthermore, patients in an early tumor stage can often be treated with therapies that have fewer side effects. However, the extent of the benefits offered by screening actually depend on the type of cancer involved. For example, the benefit of certain examinations for early detection of breast cancer, bowel cancer and cervical cancer is scientifically proven and widely recognized by experts. For this reason, personal invitations to these examinations and information are sent to the people entitled to claim them.
Drawbacks of cancer screening
Along with the aforementioned advantages, cancer screening can also be associated with drawbacks and stresses and strains.
- While an early diagnosis does increase the chances of healing, it does not provide any guarantee of this.
- A cancer may have developed so quickly that it will cause sudden symptoms between two exam appointments.
- The examination itself can have risks such as complications during the colonoscopy.
Also, no method is 100 percent reliable. This means that healthy people may be mistakenly diagnosed as sick and sick people as healthy.
- It is quite common for a suspicious test result to be exposed as a false alarm (“false positive” result). Such false positive results involve irksome and unnecessary follow-up tests, for instance taking a tissue sample (biopsy).
- If a tumor is not discovered by a test, this is called a “false negative” test result. Those affected wrongly think that they are safe.
Overdiagnosis and overtherapy – what does that mean?
Thanks to early detection screening, slowly growing tumors can also be discovered. They do not cause symptoms and usually do not reduce life expectancy or limit the quality of life of those affected. The discovery of such a tumor as a result of early detection screening is called overdiagnosis. Its treatment – with all the associated complications and risks – is regarded as overtherapy. Unfortunately, it is not possible, as a rule, to predict with the currently available examination methods whether a tumor will grow slowly or aggressively in a patient.
Important: Due to these potential drawbacks, it is important to be well informed before availing of a screening for the early detection of cancer. Neutral information that is based on scientific evidence and easy to understand can help with the decision for or against cancer screening. Participation in cancer screening is always voluntary.
Where can I find more information?
If you would like to know which examinations for cancer screening and prevention you are entitled to, you can, for instance, get in touch with your family doctor.
Furthermore, there are websites that offer comprehensive information about these topics. These include:
IQWiG: health information on screening
Federal Ministry of Health (Bundesgesundheitsministerium): early detection of cancer for men and women
Cancer Information Service (Krebsinformationsdienst): screening and early detection of cancer
German Cancer Aid Foundation (Stiftung Deutsche Krebshilfe): early detection of cancer
Mammography Board (Kooperationsgemeinschaft Mammographie): information about the Mammography Screening Program
Medical Service of the Central Association of Health Insurance Funds (Medizinischer Dienst des Spitzenverbandes Bund der Krankenkassen e.V.): IGeL Monitor
If you need personalized information, you can also make direct contact with Cancer Information Service doctors by dialing the freephone number (0800) 420 30 40 or sending an email to krebsinformationsdienst@dkfz.de.
- Gemeinsamer Bundesausschuss. Früherkennung von Krebserkrankungen. Aufgerufen am 28.02.2025.
In cooperation with the Cancer Information Service of the German Cancer Research Center (Krebsinformationsdienst des Deutschen Krebsforschungszentrums).
As at:

